HCG at 6 weeks of obstetric pregnancy - normal
- HCG norms
- HCG norms for IVF
- About analysis (video)
The human body has a specific hormone called human chorionic gonadotropin.
It has the ability to be actively produced after fertilization has occurred and pregnancy has begun to develop. It is produced exclusively by the cells of the embryo - chorions, after the fertilized egg has attached to the uterine wall.
There are accepted hCG norms for obstetric weeks, which indicate the onset of an “interesting” situation, as well as the correct or abnormal development of the fetus.
Human chorionic gonadotropin really plays an invaluable role. For example, during the first three months of pregnancy, it is responsible for the production of sufficient amounts of progesterone and estrogens. In addition, hCG affects the cells that produce testosterone, which is responsible for the formation of male sexual characteristics.
HCG norms
The hCG level for obstetric weeks of pregnancy makes it possible to approximately calculate the date of future birth, since the indicators determine the approximate date of conception. Already after the first days of fertilization, when taking a blood test, an increased level of human chorionic gonadotropin can be noted.
Of course, you can use a standard test, but the result may be false, since the hormone content in this case changes in the urine and not in the blood, and it is almost impossible to determine the exact date of conception if the woman herself does not know it. Many people are interested in how hCG is calculated, from conception or by obstetric weeks. It is customary to calculate the day of pregnancy using obstetric weeks (starting from the last day of menstrual bleeding), and the norms themselves are calculated from conception.
HCG norms for natural conception
It is necessary to donate blood to determine the level of human chorionic gonadotropin in the first days of a missed period, or no later than two weeks, otherwise the test results may be erroneous. Blood from a vein should be donated in the morning on an empty stomach, and to obtain the most accurate data, the test must be taken several times with an interval of a couple of days.
The hCG level is measured in honey/ml; the norm for natural conception will be as follows:
- The first 7-14 days from conception or 3-4 obstetric weeks - 25-156;
- 14-28 days from conception or 4-5 obstetric weeks - 101-4870;
- 28-35 days or hCG norm at 5 obstetric weeks – 1110-31500;
- 35-41 days from conception or hCG norm for 6 weeks of obstetric pregnancy – 2560-82300;
- 41-48 days or 7-8 weeks of pregnancy – 23100-151000;
- 48-55 days from conception or 8-9 weeks of pregnancy – 27300-233000;
- 55-62 days from conception or 9-10 weeks of pregnancy – 20900-291000.
In the future, with the development of a normal pregnancy, without any anomalies or deviations, the level of human chorionic gonadotropin will gradually decrease.
HCG during obstetric weeks in the first stages doubles every two or three days, which is considered natural and normal.
If the indicators decrease during this period, then doctors should consider the need for maintenance therapy to preserve the fetus, or make sure that the egg has implanted in the uterine cavity and not in the tube.
It is also worth noting that hormone levels increase significantly during multiple pregnancies. So, for example, if a woman is carrying at least two children, then her CHF level at 5-6 obstetric weeks will be in the range of 2220-164600.
In situations where dynamic studies confirm the normal development of the fetus, but the level of human chorionic gonadotropin decreases before the onset of 8-9 weeks, it is worth double-checking the established timing of pregnancy; it is possible that an error was made in them.
HCG norms for IVF
If a woman for some reason cannot get pregnant on her own, doctors prescribe her hormonal therapy, which provokes the onset of ovulation. If sexual intercourse is successful and sperm motility is good, pregnancy occurs in most cases after such treatment.
Table of hCG norms for artificial insemination
It follows from this that the level of their concentration in the blood may be overestimated, which distorts the real picture and can give a false-positive result when conducting a standard pharmacy test. HCG norms during pregnancy by obstetric week, in the case of in vitro fertilization or stimulation, will differ:
- Pregnancy 3-4 weeks – from 10 to 170;
- Pregnancy 4 weeks – 170-27300;
- The hCG level at the 5th obstetric week of pregnancy after IVF is 27300-74000;
- The hCG level at the 6th obstetric week of pregnancy after IVF is 74000-128200.
Subsequently, the indicators, as with natural conception, increase until 8-9 weeks, after which they begin to gradually decrease. As for multiple conceptions, there are no exceptions, and the hCG level will be approximately two times higher than the norms determined for women who became pregnant artificially.
About analysis (video)
Source: https://Pro-MD.ru/ivf/other/hgch-na-6-nedele-akuserskoj-beremennosti/
HCG level during pregnancy - table of norms by week and interpretation of blood test results
The fact of conception is clarified by examining biological fluids. A portion of blood is collected at the clinic, but urine is important for using the home test. The level of hCG changes cyclically over the weeks of pregnancy, which is why the viability of the fetus is determined in this way.
It is known that human chorionic gonadotropin is a natural hormone that is supposed to be produced by the chorion if a viable egg has already attached to the wall of the uterus.
At first, its concentration is moderate, but as the period increases, it begins to change cyclically, and upward.
It is recommended to take a blood test so that the doctor can confirm the birth of a new life and organize a diagnosis of the mother for hidden infections.
In the first trimester, the hormone begins to increase rapidly, reaching its maximum concentration at 8-9 weeks of obstetrics. Then its systematic decline begins, characterizing the stable dynamics of the baby’s development.
If a high hCG value is recorded during pregnancy, for example, at 13 weeks or more, this is a suspicion that there is a pathology fraught with danger for the baby.
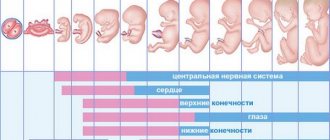
In modern gynecology, the stages of fetal development throughout the entire period of formation of the body are recorded using this indicator.
In order to draw conclusions about the intrauterine health and condition of the expectant mother, it is important to know the decoding of human chorionic gonadotropin in the blood.
For clarity and accessibility, hCG indicators during pregnancy by week are listed in a table, which helps the young lady control her condition.
It is important to discuss any discrepancy with the norm with a gynecologist; hormonal correction is immediately introduced. A table with a correctly performed calculation is detailed below.
| Obstetric weeks | HCG norms by week of pregnancy, IU/l |
| 5-6 | 50 000-200 000 |
| 7-8 | 20 000-200 000 |
| 9-10 | 20 000-95 000 |
| 13-14 | 15 000-60 000 |
| 15-25 | 10 000-35 000 |
| 27-38 | 10 000-55 000 |
Such a table is shown as a note to every patient who is expecting a new addition to the family soon. If there is a delay in menstruation, analysis and a home test can determine the fact of successful conception, and in the first case, the approximate period of the interesting situation. Any lady planning to procreate should know how and when to donate blood for hCG.
HCG by days from conception
When preparing for motherhood, it is useful to find out the pattern of hormone growth from the moment of successful fertilization of the egg. The cause of hormonal changes is considered to be the formation of the chorion, a failure in the concentration of progesterone.
By studying hCG day by day from conception, you can determine the real condition of the fetus. If the hormone begins to increase, implantation has taken place with a favorable outcome, or natural fertilization has gone well.
In cases where it drops rapidly, doctors do not rule out intrauterine implantation of the fertilized egg or the non-viability of the embryo.
| Day from the moment of successful fertilization of the egg | DPO level (normal indicator), IU/l |
| 8 | 1,4 |
| 10 | 1,9-13,1 |
| 11 | 8-35 |
| 13 | 33-91 |
| 14 | 57-140 |
| 16 | 155-430 |
| 18 | 740-1030 |
HCG for ectopic pregnancy
This is a death sentence for women who dream of motherhood, which becomes a real tragedy. The question arises: does hCG indicate an ectopic pregnancy? The answer is strictly affirmative.
The hormone is detected, so the test strip gives a positive result from a home test. However, in reality, the patient has no idea how much the hormone should be.
With ectopic attachment, its level is much lower, and the anomaly is determined only after the appropriate analysis.
HCG level during frozen pregnancy
If such a problem occurs, it may not be immediately identified. Several days pass until the doctor confirms the death of the fetus.
The hCG level during a frozen pregnancy must be re-checked several times before removing the embryo from the uterine cavity. Each time the reading obtained will gradually decrease, although ideally it should increase rapidly.
Calculating the anomaly will not be difficult, and the patient will undergo immediate surgical intervention.
How should hCG rise?
It is necessary to monitor hCG levels during pregnancy. Frequent laboratory tests make it clear that the process of intrauterine development of the fetus occurs without mutations.
Every day the level of hubbub gradually increases, but its increase is especially noticeable during multiple pregnancy. It is on the presence of such a blood component that home testing methods for interesting situations are based.
If you are interested in how hCG increases during pregnancy by day, you can get detailed information from approved tables.
Elevated hCG during pregnancy
Any deviations of the indicator from the norm must be promptly identified and eliminated. Before donating blood for hCG, it is important to consult a gynecologist for advice.
The result is due to the correct execution of the study in the laboratory, for example, material from a vein should be taken a couple of weeks after the expected process of ovulation, only on an empty stomach. There are several such nuances and preparatory activities.
If the laboratory test is organized correctly, but there is still a high level of hCG in the early stages, the reasons for the deviation are as follows:
- toxicosis at an early stage;
- incorrect calculation of the deadline;
- multiple pregnancy;
- Down syndrome in an unborn baby;
- diagnosis of diabetes mellitus in the body of a future mother;
- free use of certain groups of medications.
Pregnancy 6 obstetric weeks - where is the embryo? | Page 11
542 replies
Last - April 01, 01:00 Go
Lydia
Hello girls. Reading you, I involuntarily wanted to tell my story, perhaps in order to support those who are diagnosed with a frozen pregnancy in the early stages. According to my calculations, I was already about 8, if not more, weeks pregnant when the doctor gave me an ultrasound reading of 3 weeks.
He said that most likely the pregnancy is frozen, he advised me to wait for 2 weeks, if a miscarriage happens, then it will happen, if not, then come for a repeat ultrasound. Two weeks of waiting for God knows what, but the miscarriage did not happen. And at the repeat ultrasound they said that the fetus was 30mm, a heartbeat could be heard, the term was 8 weeks.
How can this be, I asked, strange arithmetic, in 2 weeks the fetus has developed 5 weeks. The doctor said that this was how implantation took place in the wall of the uterus. I was diagnosed with fetal growth restriction throughout my entire pregnancy, and I gave birth 2 weeks later. I think that because of my problems with my cycle, I just got pregnant later.
Now my son is 11 years old, he is an absolutely normal child and even one of the strongest students in the class.[/quote
Nastya
Girls, at 6.5 obstetric weeks, the doctor also did not see the embryo or heartbeat on my ultrasound. But the doctor reacted calmly during the consultation, hCG at 4 weeks corresponded to the norm. The next ultrasound was done only at 12 weeks.
The baby was found, and the heart is beating as it should. It’s just that the ultrasound was done for the first time by a not very professional doctor... So many worries about her...
In general, the doctor at the housing complex said that it is better not to do an ultrasound before 8-9 weeks, so that there is less worry.
Olga
Girls, I was diagnosed at the LCD at 7-8 weeks, they sent me for an ultrasound, the ultrasound revealed that there was a fertilized sac, there was no embryo and the term was 4 weeks. I also had pain in the lower back and lower abdomen. I stayed at home for 1.5 weeks and went for an ultrasound to another doctor. The driver herself was stuck in traffic jams in the morning, was late for the appointment, and was nervous.
On the ultrasound, a blue pulsating point was clearly visible. The doctor turned the monitor towards me and asked who said that the embryo could not be seen and the heartbeat could not be heard? She said that the doctor had a gastrointestinal tract. “What is this?” he asked. It’s either the volume or something else. something, but I myself saw this pulsating point and heard the heart beating.
Now I’ll go to the residential complex, register, and go to the pyronotal center in another city for examination.
I don’t believe our doctors, bastards! During my first twin pregnancy, this uzologist, who didn’t see anything, sent me for cleaning at 19 weeks, said that the twins were conjoined and needed to be cleaned, thanks to my mother, she took me by the hand and took me to another city, and they even counted the fingers on their hands (now these twins are 17 years old). Don’t write off getting cleaned, wait another 2 weeks, go to all the doctors.
Evgeniya
Girls! Please reassure me(((at 6.6 obstetric weeks I started to have brown discharge, I ran to the hospital. They left me for safekeeping. They did an ultrasound and said that there was a fertilized egg, but no embryo!!! I’m all upset... Something like that ??? Maybe someone has had this happen? Maybe everything will be fine??? And the embryo will appear???….
Evgeniya
Girls! Please reassure me(((at 6.6 obstetric weeks I started to have brown discharge, I ran to the hospital. They left me for safekeeping. They did an ultrasound and said that there was a fertilized egg, but no embryo!!! I’m all upset... Something like that ??? Maybe someone has had this happen? Maybe everything will be fine??? And the embryo will appear???….
Guest
Hi all! I went for an ultrasound today, the due date was 4-5 weeks, the PU is 6 mm, but there is no embryo, a control ultrasound in 2 weeks, but I can’t imagine how I’ll wait, a week ago my stomach hurt like during my period, now it’s just dragging, there are no other changes ( no nausea or breast swelling). So I’m thinking about waiting or still trying to go to another uzist?
Guest
That’s right! they used to give birth in a furrow and didn’t think twice about it, but now...
nata
I had an ultrasound yesterday, 6 weeks due, if you count by the last period. The fertilized egg is not of the correct shape and the embryo is not visible, they told me to come back for a repeat ultrasound in 10 days.
I’m very afraid ((This is my 3rd pregnancy, during the first pregnancy I didn’t have any problems, a healthy daughter was born, the second one was ectopic, I really hope that everything will work out during this pregnancy and we will see our baby.
NN
Probably, everything has already been resolved for the author, but I will say that the other day I had the same thing... I came for the 1st ultrasound, according to the monthly period it was almost 7 weeks, on the ultrasound there was 1 fertilized egg, a sac, but there was no embryo or heartbeat , came 10 days later for a repeat ultrasound - everything is fine! so if anyone has a similar situation, don’t worry