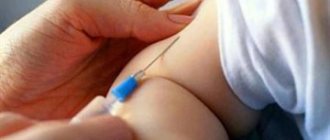
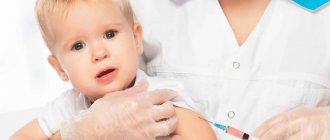
(Another useful site - experts on vaccinations)
If for some reason your child has not been vaccinated in accordance with the vaccination schedule, then most likely his body is not sufficiently protected from dangerous infections and continued immunization may be required.
missed hepatitis B vaccination
BCG vaccination schedule was violated
missed the DPT vaccine
Missed polio vaccination dates
missed vaccination against measles, rubella or mumps
If for some reason your child has not been vaccinated in accordance with the vaccination schedule, then most likely his body is not sufficiently protected from dangerous infections and continued immunization may be required. However, each vaccine differs in its antigenic composition, the intensity of the reactions it causes in the body and the duration of action. Therefore, the question of what the further timing of vaccination is is always decided individually, taking into account the state of the child’s immune system, the diseases he has suffered and the type of vaccines. As a guide for constructing a further vaccination schedule, the following general recommendations can be given, which consider violations of vaccination deadlines separately for each category of vaccines.
Hepatitis B
·If the first vaccination against hepatitis B is missed, that is, it was not performed in the first 12 hours after the birth of the baby, then you can start vaccination on any subsequent day and then follow the standard schedule - the second vaccination is given a month later, and the third after another 5 months.
·If you missed the hepatitis B vaccination, which is performed, according to the vaccination calendar, a month after birth, then it can be performed a maximum of 4 months after the first one. Moreover, the shorter the interval, the more reliable immunity will be formed. If more than 4 months have passed since the first vaccination, then the administration of vaccines is usually continued as if the vaccination schedule had not been disrupted, but in this case there is a high chance of insufficient immunization. If the doctor doubts the effectiveness of further vaccination, then it may be necessary to determine antibodies to the hepatitis B virus in the child’s blood, with a mandatory quantitative study.
·If you miss the third hepatitis B vaccination, you do not have to worry about a decrease in the effectiveness of vaccination for 18 months after the first vaccination. This is the maximum period of time after which an analysis for the concentration of antibodies against hepatitis B will most likely be required to complete the course. In some cases, when sufficient immunity has not been formed even after completing the course of vaccination, additional vaccination may be required.
BCG
·If the timing of BCG vaccination is violated, then the tuberculosis vaccination is given in the fourth month of life. Before vaccination, a Mantoux test must be performed and vaccination is carried out only if a negative result is obtained. A positive test may mean that the child has already encountered the tuberculosis pathogen and may be infected. This is an indication for further, more detailed examination. The timing of the vaccination is due to the fact that during the first 3 months of life, immunity has not yet been formed enough to give an adequate response to the introduction of tuberculin, which is used in the Mantoux test, and the reaction may be false negative. If you have not yet been vaccinated, but it is known that the child has been in contact with a patient with tuberculosis or a carrier of Koch's bacillus, then low doses of anti-tuberculosis drugs are prescribed and, after completing the course of preventive treatment, the Mantoux reaction is examined. If the test is positive, treatment is continued, and if the test is negative, vaccination is performed, followed by isolation of the child for a week. For normal formation of post-vaccination immunity, at least a month must pass between the BCG vaccination and other vaccinations.
DTP
·If you missed the DTP vaccination, which according to the vaccination calendar is performed at 3 months, then you can start the vaccination course at any time before the age of 4 years. After 4 years of age, the administration of domestically produced vaccines with a pertussis component is not allowed, but the French analogue Tetracoc (with an anti-poliomyelitis component in the composition) can be used. From 4 to 6 years of age, vaccination is done with the ADS vaccine, and after reaching 6 years of age, ADS-M is used. These are vaccines without pertussis components, the latter contains reduced dosages. If a child has had whooping cough, and you have not yet received a single DPT vaccination, then vaccination with DPT toxoid is carried out (two vaccinations with a month's interval and one revaccination after a year).
· Violation of the timing of vaccination of the second DTP vaccination does not entail a repetition of the entire cycle - the administration of vaccines continues as if the schedule had not been lost, maintaining an interval between vaccinations of 30 days. If by this time the child has had whooping cough, then he is no longer given DTP vaccinations; instead, ADS is used, and after 9-12 months the ADS is repeated
·If the third DPT vaccination is missed, it is performed regardless of the omission. If a child who has already been vaccinated twice with DTP has had whooping cough, the course of vaccination is not continued and is considered completed. Revaccination is carried out with ADS, after 9-12 months. As already mentioned, from the age of 4, vaccines without a pertussis component are administered. In order to have time to fully vaccinate a child against whooping cough, sometimes it makes sense to perform the first DPT revaccination, maintaining only the minimum permissible interval - 6 months.
Polio
·If the first polio vaccination is missed, children under 6 years of age are vaccinated twice, with an interval of 30 days. For children over 6 years of age, the vaccine is administered once.
·If the second polio vaccination is missed, vaccination is not started again, but continued, despite the extended interval. The current vaccination calendar is built taking into account the use of OPV (live polio vaccine), but it is acceptable to replace it with IPV (an inactivated vaccine, more effective).
·If the third or fourth vaccination against polio is missed, then the tactics are the same as if you missed the second vaccination. It is important that before reaching 2 years of age the child is vaccinated 5 times with OPV or 4 times with IPV. When using vaccines together, the total number of vaccinations should not be less than 4.
Measles, rubella, mumps
·If your vaccination schedule has been thrown off track and you have missed your first measles, rubella or mumps vaccination, it is best to get it as soon as possible. According to the vaccination calendar, vaccination against these infections is carried out simultaneously, in different parts of the child’s body, with separate syringes or by using combined vaccines containing components against several infections. It is recommended to resort to separate administration of vaccines if the child has already had any of the listed infections, against which the creation of specific immunity is no longer required. Even if the timing of vaccinations has been significantly shifted, subsequent revaccination is carried out at the age indicated in the national vaccination calendar.
·If revaccination against measles, rubella or mumps is missed, the vaccine is given at any appropriate time, trying to create immunity before the child enters school. If for some reason vaccinations against rubella, mumps and measles are performed in the form of single-component mono-vaccines, then the recommended interval between their administration should not be less than a month. Otherwise, there is a risk that the second vaccine will be inactivated by immune cells produced in response to the first vaccine.
·If vaccination against rubella, which is given to girls during adolescence, is missed, it is done as soon as health conditions allow. The vaccine can be done at any age unless pregnancy is excluded.
Hepatitis B
In the vaccination calendar, the hepatitis B vaccine comes first: it is given to the child during the first day in the maternity hospital. Hepatitis B is an infectious disease that causes severe liver damage. The second vaccination is carried out at 3 months, the third at 6 months.
Is it worth vaccinating your baby right in the maternity hospital?
Doctors have differing opinions on this matter. Many people believe that it is not advisable to vaccinate in the first hours of life, since the newborn still has a very poor immune response and vaccination may turn out to be pointless - the child will not develop immunity against hepatitis B.
· It is more reasonable to postpone the first vaccination to a later time, for example, you can do it at 3 months, then vaccination will be carried out according to the scheme: 3-6-9 months.
·Children are vaccinated according to a special scheme if their mothers are carriers of hepatitis B or there are people in the family suffering from this disease. Babies must be vaccinated in the first 12 hours after birth, the second vaccination is carried out at the age of 1 month, the third at 6 months, and the fourth at 12 months.
· The vaccination is done intramuscularly in the anterior lateral part of the thigh, and after 3 years - in the shoulder.
·Vaccination is usually tolerated quite easily by the child. In some cases, there may be a slight rise in temperature, thickening, and redness at the injection site. No special preparation is required for vaccination.
·For hepatitis B there are single vaccines (Combiotech, Euvax B, Engerix B, etc.) and combined ones (for several diseases).
It is advisable that intramuscular administration of vaccines to young children should be carried out in the anterior lateral part of the thigh. When the vaccine is administered into the buttock, complications often occur (there is a risk of getting into the subcutaneous fat, which leads to swelling); the nerve trunk can be damaged, and there is a smaller immune response. For older children, injections are given in the upper third of the shoulder.
Answers to frequently asked questions about DTP vaccination
What is the DPT vaccine for?
DTP is an adsorbed pertussis-diphtheria-tetanus toxoid. This is a vaccination against 3 diseases: whooping cough, diphtheria and tetanus.
Should I give DPT to my child?
The decision about whether or not to get the DPT vaccine is made by parents. They can refuse any vaccination in writing in accordance with Article 5 of Federal Law No. 157 and Order No. 229 confirming it. But an unvaccinated child can become infected and suffer severe diseases. In addition, you will have problems entering public educational institutions.
After DTP, the child is capricious and does not eat
There is no need to worry about this; such a child’s reaction on the first day after vaccination is quite normal. The very next day his general condition returned to normal. Give him as much water as possible and put him to the breast more often.
A rather rare exception is the incessant cry of a child (monotonous, high-pitched cry). In this case, you need to call a doctor at home so that he can help you choose a way to reduce the vaccine reaction. Further DTP vaccinations are contraindicated for such children.
How to relieve pain for a child after DTP?
If the child is very worried, and the injection site is very painful, then you can give the baby Nurofen for children; it not only reduces the temperature, but also has an analgesic effect.
Is it possible to wet the DTP vaccine?
It’s possible, there’s nothing wrong with it, you can’t comb or rub it.
Is it possible to bathe a child after DPT?
In the first two days, swimming is not recommended due to the possibility of a rise in body temperature. You can wipe the baby with wet wipes and rinse under running water. But if the temperature does not rise on the first day, then on the second day you can already bathe the baby.
Is it possible to walk with a child after DPT?
Due to the fact that in most cases the baby has an increase in body temperature, walking in the first two days is not recommended, but if the temperature is within normal limits, then you can take walks in the fresh air.
Read more about when you can walk and swim after vaccination in the article on our website.
Tuberculosis
A child is vaccinated against tuberculosis in the maternity hospital in the first 3-7 days. Contraindications to vaccination are low body weight (less than 2000 g), intrauterine infection, hemolytic disease of the newborn, purulent-septic diseases, severe damage to the central nervous system.
·If the child was denied vaccination in the maternity hospital, it can be done later (preferably before 6 months). Please note that if you are going to vaccinate a child older than 2 months, you will first need to do a Mantoux test. This is necessary to find out whether the child is infected with the tuberculosis bacillus - then vaccination will be contraindicated for him.
·Vaccinations against tuberculosis are given only in a medical facility; Doctors visiting homes do not have the right to vaccinate children against this disease.
·Vaccination against tuberculosis is always carried out separately from other vaccinations.
·Every year, a child is given a Mantoux test to determine whether he is infected with tuberculosis. If the baby was vaccinated already in the maternity hospital, then the Mantoux test is given to him for the first time at 1 year.
· The vaccination is given to children intradermally - in the area of the left shoulder, at an older age - under the shoulder blade.
·Two vaccines are used against tuberculosis - BCG and BCG-M (light version).
· Revaccination is carried out at 7 years of age.
What to do to avoid the negative consequences of vaccination?
The negative consequences of immunoprophylaxis cannot be guaranteed to be avoided; this applies to any vaccines.
But you can reduce the likelihood of side effects. To do this, you need to prepare your baby for vaccination in a certain way. It is also important to follow a number of rules during the post-vaccination period.
Preparing the baby
Preparation is an important point in carrying out immunoprophylaxis. A completely healthy child should be vaccinated.
If the body is weakened, then vaccination can lead to the development of whooping cough or improper formation of protective forces. In order to understand whether the baby is ready for the introduction of DPT, it is necessary to thoroughly examine him.
Vaccination is contraindicated in the following conditions:
- nervous disorders at the progressing stage;
- increased body temperature;
- cold;
- infectious or viral damage to the body;
- epilepsy;
- encephalopathy;
- exacerbation of chronic pathologies;
- underweight;
- state of immunodeficiency;
- general malaise;
- psoriasis;
- severe allergic reaction to a previous DTP vaccine.
Preparing a child for immunoprophylaxis against diphtheria, whooping cough and tetanus consists of the following activities:
- giving antihistamines a few days before the procedure. Fenistil is good for children;
- use of an antipyretic drug on the day of the injection. It is recommended to give your child medications based on paracetamol or ibuprofen. Such medications will not only prevent the temperature from rising, but will also prevent the appearance of pain after the injection;
- do not overfeed the baby before vaccination;
- a week before the introduction of DTP, exclude from the diet all foods that can cause an allergic reaction.
Actions in the post-vaccination period
After administration of DTP, it is recommended to remain within the clinic for about an hour. During this time period, all severe side effects (for example, anaphylaxis) usually develop.
In order for the post-vaccination period to pass without complications, you should adhere to the following recommendations from specialists:
- for several days after the injection, give the child antipyretic and antihistamine drugs;
- Avoid visiting crowded places with your baby for 1-1.5 weeks. After administration of DTP, the body recognizes the antibodies and begins to fight them. During this period, the immune system weakens and the likelihood of infection with infectious viral pathologies increases;
- do not introduce new foods into the baby’s diet;
- Do not bathe your child for a couple of days after the injection. Water procedures are especially contraindicated in cases where the house is too cold or hot, or there are drafts. Changes in temperature can cause a cold. If the water is of poor quality, then there is a risk of infection in the puncture;
- walk in the area of the forest belt, forest plantations, where there are few people. Fresh air is important for a child. Therefore, it is not worth closing it within four walls during the post-vaccination period;
- dress your baby outdoors according to the weather;
- If you suspect the development of adverse reactions, you should immediately contact your pediatrician.
Polio
For a long time, children in our country were vaccinated with a “live” oral vaccine (OPV) - it was dripped into the mouth. Unfortunately, because of this, there have been cases (albeit very rare) of vaccine-associated polio, when the disease itself developed due to the vaccine, leading to disability.
· Currently, they are trying to move away from the use of “live” vaccines, and instead use an inactivated vaccine (IPV) - it contains “killed” viruses and is not capable of causing disease. The inactivated vaccine is administered intramuscularly.
·After using a “live” oral vaccine, a child sometimes experiences stool upset for 1-2 days, and in some cases there is an increase in temperature. The inactivated polio vaccine usually does not cause such reactions.
· The polio vaccine is given at 3 months, then at 4.5 and 6 months. Revaccination is carried out at 18 and 20 months.
·The inactivated polio vaccine used in Russia is Imovax Polio. In addition, the combined Pentaxim vaccine is used (protection against polio, whooping cough, diphtheria, tetanus and Haemophilus influenzae type b).
When should revaccination be done?
After three doses of DTP, the child produces a sufficient amount of antibodies. But in the required concentration they do not last long. In order to maintain the strength of the immune system, doctors recommend revaccination.
According to the approved schedule, the fourth dose of vaccination is administered at 18 months. Then they are revaccinated at 6-7, 14, 24 years and then every 10 years. But after the age of six, a drug without a pertussis component is used - ADS, ADS-M.
It is recommended to do DTP revaccination outside of the plan in the following cases:
- when a blood test reveals a low concentration of antibodies;
- there was contact with a patient with whooping cough, tetanus or diphtheria;
- The child does not have information about the DPT revaccination performed.
Diphtheria, whooping cough, tetanus
For these diseases, combination vaccines are mainly used (that is, those that protect against several diseases at once). The first vaccination is given at 3 months, the second at 4.5 months, and the third at 6 months; revaccination - at 18 months. The vaccine is administered intramuscularly into the anterior lateral thigh or buttock. This vaccination is not always easily tolerated by the child and requires prior preparation. The heaviest component of the vaccine is the pertussis component. After vaccination, local and general reactions are possible. Local symptoms include redness and swelling at the injection site; general symptoms include malaise, fever, and in rare cases, convulsions. The reaction after the second and subsequent vaccinations is often stronger than after the first.
· Recently, vaccines have appeared that give fewer post-vaccination reactions. Good tolerability is explained by the fact that they contain an acellular pertussis component. These vaccines are foreign-made and are offered in paid medical centers.
· Before vaccinating your child against whooping cough, diphtheria and tetanus, it is advisable to prepare him: for 1-3 days before vaccination, the baby is prescribed antihistamines in age-appropriate dosages. The question of whether to give a child antihistamines on the day of vaccination and after it is decided by the pediatrician individually in each case.
·After vaccination, children may develop a fever. This usually happens 6-8 hours after vaccination; high temperature can last up to 2 days.
· Therefore, you must have antipyretic drugs at home (preferably in the form of rectal suppositories) so that you can use them if necessary.
·If after the first administration of the vaccine there was a rise in temperature to 38.5 °C or higher, then this is a contraindication to repeated vaccination with a pertussis component. Repeated vaccinations are made with vaccines without a pertussis component or containing an acellular pertussis component.
·Vaccines that protect against these diseases are DPT, ADS (without pertussis component), Infantrix, Pentaxim.
Before DTP
Preparations for vaccination should begin seven days before the scheduled date. Preparatory measures include compliance with certain conditions that are necessary to ensure a positive reaction of the child to the administered vaccine.
What not to do before DTP vaccination
On the eve of vaccination it is not advisable to:
1. Changing the child’s diet, introducing new complementary foods.
2. Use of new therapeutic drugs.
3. Visiting closed public spaces with your baby, where he can become infected with a viral infection.
4. Allow the child to become hypothermic or overheated, which can also lead to illness.
Before each DTP vaccination, regardless of whether it is the first, second or third, the above recommendations should be followed. In addition, on the day of vaccination you must:
- measure the baby’s body temperature;
— visit your local pediatrician.
Preparing for the first DTP vaccination
DPT vaccination schedule
According to the calendar of preventive vaccinations, the first DTP vaccination is performed on a baby at three months of age, the second at 4.5 months, the third at 6 months, then at 18 months, 6-7 years, and the last time at 14 years.
Before it is carried out it is necessary:
1. Visit your local pediatrician with your child, who will issue a referral for the following tests:
- general blood analysis;
- general urine analysis.
2. Perform an ultrasound examination of the baby’s brain.
3. Be examined by a neurologist, who, based on the results of an ultrasound of the brain and examination of the child, will make a conclusion and allow or prohibit vaccination for a certain period.
What to give your child before DTP vaccination
Before vaccination, your pediatrician may prescribe antiallergic medications. These include:
— Suprastin;
— Tavegil;
- Zodak;
— Zyrtec;
- Fenistil.
Taking an antihistamine is prescribed to reduce the risk of a baby developing an allergic reaction to the DTP vaccine.
More often this applies to children prone to allergic manifestations:
- rashes on the skin;
- suffering from allergic dermatitis.
The dose of the medicine is selected according to age. It is taken according to the following scheme:
■ three days before vaccination;
■ on the day of vaccination;
■ three days after vaccination.
The use of an antihistamine medication will provide a high degree of protection against possible side effects after routine vaccination of a child.
Preparing a child for the second and subsequent DTP vaccinations
Tests and a medical examination by a neurologist before the second and subsequent vaccinations are prescribed individually, according to medical indications.
If the baby’s health is fine, then it is enough to undergo an examination by a pediatrician. Antihistamines are prescribed for children who have had allergic reactions to the previous DPT vaccination:
- high body temperature;
- redness of the skin, etc.
The use of these drugs significantly reduces the negative activity of vaccination vaccines. Parents should be confident in the need to vaccinate their child. With the right psychological attitude of mom and dad, vaccinations will not bring any complications. To avoid possible risks, you must strictly follow the recommendations of your local pediatrician.
Measles, rubella, mumps
·Children are vaccinated against these diseases at 12 months and 6 years. Combination vaccines against three diseases, two-component and mono-vaccines are used. There are vaccines of both domestic and foreign production.
· Since the vaccine against these diseases is “live”, after its administration the child may experience some reactions, for example, an increase in body temperature, swelling of the lymph nodes, the appearance of a rash, a slight cough and runny nose - that is, the child seems to have suffered from these diseases in a very mild form. Typically reactions occur on days 1-2, 5-8 and 10-12.
To make it easier for your baby to tolerate vaccination, it is advisable to give him antihistamines 1-3 days before vaccination and several days after it. The pediatrician will calculate how long to give the drugs after vaccination and in what dose. Also, do not forget to stock up on antipyretic medications so that your baby’s fever does not take you by surprise.
·Combined vaccines against measles, rubella and mumps - Priorix, Trimovax and others.
How is the reaction to DPT vaccination assessed?
The district nurse visits the child on the second day after DTP vaccination to determine his physical condition. The following data is entered into the baby’s outpatient card:
— the child’s body temperature after vaccination;
- local reaction to the vaccine.
An elevated child’s body temperature of more than 39 degrees Celsius is the basis for subsequent DTP vaccinations only after preliminary preparation of the baby, that is, using antihistamines.
Other diseases
There are a number of vaccinations that are not included in the Russian national vaccination calendar, but, nevertheless, they can be done to protect the child from serious diseases. By the way, in European countries and the USA these vaccinations are included in the mandatory vaccination plan.
In our country, you will have to do them at your own expense.
· Haemophilus influenzae type b infection (Hib infection) often causes pneumonia, otitis media, meningitis and other diseases in children. It poses the greatest danger to children from 6 months to 2 years. The Haemophilus influenzae vaccine can be given at the same time as the diphtheria, whooping cough and tetanus vaccination. Three vaccinations will be required with an interval of 1-1.5 months and one revaccination, which is carried out a year after the third vaccination. If the vaccination is given to a child older than 6 months, then two vaccinations and one revaccination will be enough for him.
·Vaccine against hemophilus influenzae infection - “Act-HIB”. In addition, you can protect yourself from this disease using the Pentaxim combination vaccine.
·After 2 years of age, a child can optionally be vaccinated against pneumococcal infection that causes pneumonia (Pneumo 23), meningitis (Meningo), and chickenpox (Varilrix). In childhood, chickenpox is usually tolerated quite easily by children, but in adolescence it can be severe and cause complications.
·In addition, you can vaccinate your child against hepatitis A. Vaccination is carried out twice, the second time - 6-12 months after the first. Usually the vaccination is tolerated quite easily. Swelling and swelling at the injection site are possible. For hepatitis A, the vaccines “Havrix”, “https://www.baby.ru/pharmacy/40606-avaxim”, “Vakta” are used. There are also combined vaccines against hepatitis A and B.
Setting DPT after a year for the first time
DTP is not always done strictly according to plan. Sometimes the immunization schedule changes. In some cases, the pediatrician develops an individual vaccination plan.
There are many reasons why DPT vaccination may be tolerated:
- the child is weakened and often sick during the first scheduled vaccination;
- the baby was born premature and at three months had insufficient weight for his age, which became a contraindication for vaccination;
- the baby was outside the country for a period of three months to a year, so he could not be vaccinated with the domestic DTP;
- parents were afraid that their baby would develop serious side effects from the vaccine and waited until the child’s body got a little stronger.
Pediatrician Komarovsky recommends not to violate the immunization schedule against tetanus, diphtheria and whooping cough without good reason (serious contraindications). The doctor warns that diphtheria and tetanus are deadly diseases that occur especially often in children under one year of age.
Timely vaccination is the only option for protection against infection. But if, nevertheless, the schedule was violated, then you should take a course of immunoprophylaxis as soon as possible.
Up to four years of age, vaccination is carried out according to the standard scheme:
- the first injection is given;
- after 1.5 months the second dose is administered;
- After another 45 days, a third injection is given.
Children aged 4 to 6 years are not given DTP. For immunization purposes, a drug without the pertussis component, ADS, or its analogue with a lower dosage, ADS-M, is used. It is also allowed to use imported substitutes.
DPT is not used due to the presence of a whole-cell pertussis component in it, which is less well tolerated by children after six years of age.
Vaccination rules
·Vaccination cannot be done if the child is sick. Vaccination can be carried out 2-4 weeks after the baby has recovered.
· The interval between vaccinations must be at least a month.
·Vaccination in hot weather is undesirable.
· It is better to refrain from visiting public places with your baby before vaccination and after the administration of live vaccines.
·Before and after vaccination, it is not recommended to introduce new complementary foods to the child.
·You should not stop breastfeeding during the vaccination period.
·Members of the child’s family must be healthy at the time of vaccination.
· It is not recommended to bathe the baby in the evening on the day of vaccination.
·Parents have the right to refuse to vaccinate their child (based on the Federal Law “On Immunoprevention of Infectious Diseases” dated September 17, 1998 No. 157-FZ), but they must understand that they are responsible for the health of their child.
The body's reaction after the second and subsequent vaccinations is often stronger than after the first vaccination.
A second vaccination is not given if, after the first one, the child has the following reactions:
· shrill cry of the baby, which lasted for 3 hours or more;
·increase in the child’s body temperature to 38.5 °C and above;
· the occurrence of a strong local reaction to vaccination (redness, swelling and swelling with a diameter of more than 5 cm at the injection site).
How to prepare a child for DTP vaccination at 3 months
While in the womb, the fetus receives antibodies that protect it from disease. But when the baby is born, his body is no longer so protected; maternal antibodies last for about 2-4 months. But the immune status of different children is different and the average value is chosen for vaccination. Therefore, the first DTP injection is carried out in the third month, if there are no restrictions.
Contraindications to DPT:
- Acute diseases;
- History of afebrile seizures;
- Progressive disorders of the nervous system;
- Allergy to additional elements of the vaccine.
Children who have suffered complex illnesses, pneumonia or acute bronchitis are not vaccinated earlier than four weeks after the illness. For mild forms of acute respiratory viral infections and acute respiratory infections, the vaccine is given two weeks after recovery.
Where to get vaccinated?
·In district clinics Vaccination in district clinics in accordance with the National Vaccination Calendar is carried out free of charge. Before vaccination, the child is examined by a doctor. Information about vaccinations given is entered into the child’s card, which is stored in the clinic. The disadvantages of this option include the fact that before vaccination, you and your child may have to sit in line for a long time, and that the pediatrician has too little time to properly examine your baby. In addition, local clinics often offer not the best vaccines.
·In medical centers Here you can find better modern vaccines. The cost of vaccination will consist of the cost of a doctor’s examination (200-1200 rubles) and the cost of the vaccine itself (100-2000 rubles). If you want to contact a paid center, then carefully consider its choice - it is advisable that the medical center has a good reputation and its doctors have been involved in vaccination prevention for a long time. Information about the vaccination done must be documented - for this it is advisable to have a vaccination certificate with you (a booklet in which all information about the vaccinations given is entered).
·At home Vaccinations at home can only be done by doctors who specialize in vaccine prevention. For a child, this is the most gentle option - the baby will not have additional stress in the form of a visit to the clinic. However, it must be taken into account that vaccines must be stored under strictly designated temperature conditions. And these conditions must be observed even during transportation, otherwise the vaccine may deteriorate. Therefore, vaccination at home can be carried out only if you completely trust the doctor who will do it or the medical center in which he works. Make sure that information about vaccination is included in the vaccination certificate.
Russian national vaccination calendar
Newborns (in the first 24 hours of life) First vaccination against viral hepatitis B Newborns (3-7 days) Vaccination against tuberculosis 3 months Second vaccination against viral hepatitis B, first vaccination against whooping cough, diphtheria, tetanus, polio 4.5 months Second vaccination against whooping cough, diphtheria, tetanus, polio 6 months Third vaccination against whooping cough, diphtheria, tetanus, polio, third vaccination against viral hepatitis B 12 months Measles, rubella, mumps 18 months First revaccination - diphtheria, whooping cough, tetanus, first revaccination - polio 20 months Second revaccination - polio 6 years Revaccination - measles, rubella, mumps 7 years Revaccination against tuberculosis, second revaccination - diphtheria, tetanus 13 years Viral hepatitis B (previously unvaccinated), rubella (previously unvaccinated girls or those who received only one vaccination) 14 years Third revaccination - diphtheria , tetanus; third revaccination - polio; revaccination - tuberculosis (if you were not vaccinated at 7 years old)
On the day of DTP vaccination
First of all, the child should be examined by a pediatrician who:
- measure the baby’s body temperature;
- listen to the heartbeat and lungs;
- check your throat;
- evaluate the tests and their results;
— get acquainted with the conclusion of a neurologist;
— in the absence of contraindications to vaccination, notes in the outpatient card the appropriate permission to carry it out.
The pediatrician informs the parent about the side effects that are possible after DTP vaccination, such as:
- increase in body temperature;
- redness in the injection area, etc.
Recommendation. A children's home first aid kit should contain antipyretics (nimulid; paracetamol; nurofen) and antihistamines.
At the end of the examination, the pediatrician gives the mother permission to sign for vaccination and sends the parent and child to the vaccination office for routine vaccination. The injection is performed by a nurse intramuscularly into the baby’s thigh or shoulder, and the information about the vaccination given is entered into the vaccination card (Form 63) and the vaccination certificate.