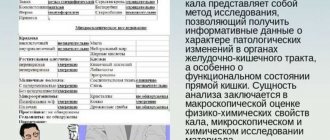
Normally, a newborn boy's testicles are already in the scrotum. If one or both testicles do not descend after birth, the condition is called cryptorchidism . Most often, this pathology occurs in premature babies (about 30% of cases) and much less often in adolescents - up to 1% of cases. The problem is that the abnormal location of the male gonads often indicates concomitant pathology and can lead to the development of serious complications: from impaired fertility to the transformation of normal cells into malignant ones.
How is surgery for cryptorchidism performed in a child?
The operation to lower the testicle into the scrotum is considered simple and is performed on average within an hour under general anesthesia.
Its essence lies in finding the testicle and further transporting it along the inguinal canal to the scrotum, after which a necessary condition will be its fixation there until complete healing. If the length of the spermatic cord is not enough, then the testicle is clipped in the extreme possible position and the operation is repeated after six months.
In some cases, the testicle at the end of the spermatic cord is completely absent, or it is considered non-viable and is removed. In this case, the operation is completed, and after a long time, when the patient becomes an adult, another operation is performed, during which the patient is fitted with a testicular prosthesis, the size, shape and density most closely matching his own.
note
After the operation, the patient remains in the hospital for at least two days. Removal of sutures is possible only after complete healing on approximately the twelfth day. During the postoperative recovery period, it is necessary to completely eliminate power loads for a period of one month.
Possible postoperative complications:
- The occurrence of hematomas, swelling and inflammation in the surgical sites.
- Testicular atrophy due to disruption of its blood supply.
- Adhesions and suppuration at the site of the surgical incision.
- Damage to blood vessels and internal organs: spermatic cord, bladder and others.
- Scrotal swelling.
- Development of hydrocele of the testicle.
- Incorrectly occupied position of the testicle.
- And in rare cases, a relapse of the disease.
On the forums you can find many reviews from parents who have encountered a disease such as cryptorchidism in children. Reviews of the operation are mostly positive, since in the vast majority of cases this procedure is quite easy and the body recovers without complications. Some reviews even include photos where you can see the appearance before and after the operation, as well as almost invisible scars.
Reviews often mention clinics located in Moscow, St. Petersburg, Novosibirsk, Irkutsk, Chelyabinsk, Krasnoyarsk and Ulyanovsk, and note the experience and competence of surgeons, andrologists and urologists.
Gender of the child. What week? | Women's magazine online - EVA.RU | Pregnancy
- I had an ultrasound. 14 weeks, they said it looked like a boy, but not exactly. Today I had an ultrasound with another doctor, I was 18 weeks pregnant, they said it looked like a girl, but not for sure. At what date did they tell you exactly and they were not mistaken?
- As far as I know, from the 20-22nd week, it seems that boyhood finally begins to form (the testicles descend or something) and you can already tell the gender, but I have a number of girlfriends, and one of them just recently gave birth - she was told the whole pregnancy was a girl (I don’t understand how in the last timing can be so wrong), I gave birth to a boy and vice versa happened with my friends. The most accurate, unmistakable diagnosis is apparently generic...
- Marvelous! Is it really true that in our time they didn’t even set deadlines?
- from 14 weeks. All subsequent ultrasounds said it was a girl. A girl was born.
- I myself am in shock, because I’m also going to have an ultrasound the other day - 20 weeks and I would like to know “who lives in the house there” ... but my friend just gave birth - a fresh example ... Maybe she, of course, came across cretinous ultrasound doctors, but when they give you an ultrasound at 8-9 months and not see... well, in general, it was a complete surprise for her, to put it mildly...
- During my first pregnancy, at 11 weeks, they said it was a girl. At 16, they confirmed it for sure. I gave birth to a girl.))) All ultrasounds were done at art-med.
- Did you yourself feel that it was a girl? Well, if you don’t take an ultrasound? I keep thinking, are there any indirect signs?? Yesterday we were at the circus - the child actively reacted only to beautiful male gymnasts and camels - in 2.5 hours there were only 4 pushes... I’m thinking... maybe there’s a girl there after all??
- Who did you do it with? What is the price?
- Of course not! People around me told me: there will be a boy! because my stomach was like a torpedo (it was elongated, like a cucumber) and my face even looked better.
- I did it at 14 weeks, it didn’t show, at 23 weeks they said it was a girl, at 27 weeks I did it (as prescribed by the doctor), the 3D showed clearly a boy, a boy was born
- At 13 weeks, Te said without any doubt that it was a boy, but I myself knew that the boy lived there. But I haven’t given birth yet)))))
- at 13 weeks, at 16, at 22 they say it’s a boy. Different ultrasound specialists on different devices. Have not given birth yet.
- The first one was set at 13 weeks. boy, you were right. With the second at 20 weeks, they were not mistaken either.
- At 11 weeks I had it done by Zinoviev, all other times I was by Mazyrko. The price depends on the period. You call, they will tell you the exact number. It’s just that it was 3 years ago. Now I’m 8 weeks and I can only tell you the exact price at the first ultrasound trimester - 1550 rub.))
- The boy told me at 12, I don’t know, everyone says he SEES everything
- The first time at 12 weeks they said it looked like a boy. Then they just confirmed it. This time at 12 they didn’t say anything, at 16 they saw the girl, at 20 they confirmed it.
- We saw a girl at 19 weeks. We'll see)
- At 11.4 Cho saw a girl))) At 17 and 21 they confirmed))) I think an experienced uzologist would not have made a mistake with your friend)))
- Does Cho look at a two-dimensional ultrasound?
- Yes, in two-dimensional, and then switches to three-dimensional))), but in two-dimensional everything is very clear)))
- By the age of 20 they usually say for sure
- The testicles descend into the scrotum immediately before birth, and in some people they may descend after birth. A classmate’s ultrasounds also “promised” a girl. She gave birth to a boy. So ultrasound at any stage does not give a 100% guarantee of gender.
- Well, our “specialists” in the residential complex may not even be able to see it at 38...))) Probably, after all, this is a matter of professionalism...)))
- Yes, the only question is where the uzist’s hands come from)))
- I was told at 16 weeks and at 26 that it was a girl) I don’t know yet... I’m still going)))
- at 14 weeks, the uzist woman said with such confidence that it was a boy, he said the genitals were visible so well, just like a boy, then 2 times at a later stage they said it was a girl, and in the end, a girl was born!!!
- Basically, by 30 weeks you can see whether the testicles have descended into the scrotum or not
- Good ultrasound specialists don’t make mistakes, they never made a mistake for me at the Center, but in the consultation they tried to call boys girls
- They were able to tell me at 22/23 weeks, before that it wasn’t clear
- Yeah, my friend in the residential complex was always saying that it was going to be a girl... And a boy was born -)
- Oh, well, Te, it’s just that a priori is never wrong, go to him and you’ll know for sure
- We were told at 13 weeks that it looked like a girl, and already at 20 weeks they told us it was clearly a boy!!! It’s already 37 weeks and they keep saying it’s a boy!
- At 13, we were “very inaccurately” guessed to be a boy. At 15, the umbilical cord lay beautifully in an interesting place. Tomorrow we go at 21.5 - we hope they will already tell us!
- I was told it was a boy at 14 weeks and a girl at 18 weeks. At 23 a boy. A boy is born!
- At 12 weeks, the Center said “80% boy.” The percentages were confirmed!
- Girls, what is Cir? Center for Immunology and Reproduction? or laboratory? I have to do an ultrasound the day after tomorrow - I want to go to good specialists.
- Center for Immunology and Reproduction. There is a good ultrasound at Tretyakovskaya, I haven’t been to other branches, but probably also.
- I’ll try to make an appointment tomorrow for the day after tomorrow, but I don’t think I’ll probably be able to do it... but can anyone else tell me where I can get an ultrasound done? I have to do an ultrasound the day after tomorrow, but where I signed up I understand that I’m not ready to go... and I wouldn’t want to do it anywhere, because I want it to be done well.
- My friend signed up there in a short time, and once she even got to Te without an appointment! So give it a try
- At ART-Med, at 14 weeks of pregnancy, they said that it was 99.9% a girl, then the ultrasound confirmed only a girl. As a result... we have a daughter. I know that they looked not only at the genitals.
- A couple of hours before giving birth. I didn’t turn around and that’s it! They couldn't say anything about who was there.
- The ultrasound already said 12 weeks)
- at the 10th week in the Center they said that it looked like a boy, at 16 weeks in the same Center they definitely saw that it was a boy))
- After the eldest was a boy at 12 and 20 weeks, and then suddenly became a girl at 30, I don’t believe in early gender determination. I will find out (at the request of the family, I would like a surprise myself) at 30 weeks.
- Quote: “In general, the testicles descend closer to full term, and only in some boys a little earlier.”
- And here are more quotes from the same page: “At 12 weeks, the ultrasound doctor can make an assumption regarding gender, sometimes it is a little more accurate than 50/50.” How accurate are the results of determining the sex of a child in the first trimester of pregnancy? Experienced ultrasound specialists can determine gender by measuring the angle of the genital tubercle. At week 11, the error rate is approximately 50% (out of 100 boys, 14 are accurately gendered); at week 14, gender determination is more accurate.”
- quote from the pregnancy calendar “25th week: this week the genitals are finally determined. In boys, the testicles descend into the scrotum; in girls, the vagina develops.”
- Apparently, there are so many doctors - so many opinions. For me personally, only at the last scheduled ultrasound (I think at 37 weeks) it was said: “The testicles have already descended into the scrotum.” This was not the case at the penultimate ultrasound.
- where did they do the ultrasound? It’s just that there are inexperienced ultrasound technicians - especially at 12 weeks - it is already possible to determine the sex of the child with high accuracy if the ultrasound technician is experienced and knows all the pitfalls. In the early stages, they look not specifically at the genital organs, but at “at what angle is the genital tubercle located” and so on. -In order to avoid mistakes, an experienced specialist is needed.
- It’s just that the specialist doesn’t say whether he’s experienced or not.
- That is, Te is an experienced ultrasound specialist and he sees everything in the corners?
- Apparently, it’s different for all boys. With my youngest son at 30 weeks, Te said that the testicles were already in the scrotum
- you know, in general, it doesn’t matter to me what gender the child is and it is important that the ultrasound specialist notices the problem in time, and not at what angle the tubercle is at. So I don't bother with it anymore. I had it done by an experienced ultrasound specialist in Healthy Generation.
- If Te at 15.5 weeks said it was a girl, can you believe it? Really, I really want him to be right!
- Everyone here writes that they are not mistaken! Maybe he is a psychic and not an uzologist?!))))
- Ha!!! Maybe it’s true, I’ve never read so many reviews about anyone else!!!
- Well, he was just a very professional, attentive, explained everything, told me everything!
- He is mistaken, there have been cases here on the forum several times. But the errors were mostly up to 13 weeks.
- Yes, he is wrong up to 13 weeks, he himself says that up to 13 is not entirely accurate. And then, he says, it’s the same as putting a boy and a girl in front of you, can you confuse them?)))
- At 36 weeks
- Then he could predict gender from conception
- Yes, and at 12+4 he confidently told me, well, I don’t know, of course, we’ll wait for the next ultrasound, and he’s really a very confident doctor.
- He told us in such a tone that I even hesitated to ask “but exactly?”
- Yeah, but I still asked him again, he said, believe it or not, I see a boy.
- At TsIR, at 12 weeks, Blokhina told me for sure that it was a girl, and at the same TsIR, Ivanova at 16 weeks said that it was 200% a boy. So I’m sitting and thinking... who’s there?
- definitely the one “more to the right”, whose ultrasound is later. At 12 weeks, I would only trust Te to determine the sex, and even then not with certainty
- I’m also inclined to believe the second ultrasound, but I still have doubts...
- At week 11, my gynecologist saw a boy, but the ultrasound doctor who was nearby did not see anything))). Now my son is almost 1.8 years old)))
- At 12 weeks they slightly noticed a boy (very hesitantly), and at almost 22 weeks they firmly said that it was a girl. I believe the second ultrasound, I don’t even think about the 12-week one, because... whatever one may say, it’s too early to determine the deadline
- With the second one at 13 weeks they said it was definitely a boy. We were not mistaken. With the first at this stage, they first saw a girl, and by 5 months a boy.
- I was 13 weeks pregnant. at the Central Research Institute, they said 90% was a boy, I haven’t done an ultrasound yet
- at 12 weeks 80% said it was a boy, at 18, 22 and 27 they confirmed
- At 16 weeks they predicted a girl, but at 22 weeks they said it was definitely a boy. In the end, boy!
- They also look at the ribs (count), and men seem to have 1 less?
- is this the one he once gave to Eve?
- Those. at 11.5 weeks I saw the gender correctly all 3 times
- What are you doing?????
- I only read about the fact that ribs are counted here on Eva this week, a girl was talking about how she had an ultrasound done and the doctor determined the gender based on the ribs and counted them.
- Well, I know that forensic experts somehow determine the sex of a skeleton based on the ribs. but they don’t seem to count them, namely some features in the structure, something like the chest is narrower. Maybe the child is also being looked at according to some type. after all, both have the same quantity
- So I think there can’t be different numbers... There must be an even number, because they are symmetrical. The girl (who was identified on the ultrasound) must have misunderstood the doctor.
- I found on Wikipedia “A person has 12 pairs of ribs, adjacent to the vertebrae at the condyle.”
- the first time at 13, the second at 18.
- I also saw on Wikipedia that there are 12 pairs. but women have narrower chests than men. maybe according to this parameter? but it seems to me that the ribs are definitely not being counted.
Source: https://eva.ru/pregnancy/messages-2644065.htm
Married couples who are preparing to become parents of a son or have recently become parents often wonder when a boy’s testicles descend. It is not surprising that the sexual development of the baby worries mom and dad, because undescended testicles (cryptorchidism) is a common pathology among newborn boys, which can lead not only to a cosmetic defect, but also to male infertility.
By asking mothers of boys you know or by looking at the forum of young parents, you can see that the timing of testicular drooping in boys varies on average from 0 months to a year. So, when do boys' testicles normally descend?
Testicular descent in boys: how does it happen?
The formation of the reproductive system in boys begins at 6-7 weeks of intrauterine life, when the rudiments of the fetal testicles - the reproductive cords - appear.
Starting from the 3rd month of pregnancy, cells that produce the male sex hormone – testosterone – are formed in the fetus’s body.
In the period of 12-20 weeks of intrauterine life, under the influence of hormones, the formation of the external genitalia, prostate gland, urethra, and epididymis occurs.
The period when boys' testicles descend occurs in the second half of the gestational age, closer to 30 weeks of pregnancy. The testicles in boys descend due to a combination of several factors:
- exposure to intra-abdominal pressure;
- producing sufficient amounts of testosterone;
- developed ligamentous apparatus of the testicles.
IMPORTANT! The process by which boys' testicles descend into the scrotum is normally completed no later than six weeks after birth, in some cases within the first year of life.
Two stages of testicular descent in boys:
- prolapse in the abdominal cavity;
- passing through the inguinal canal directly into the scrotum.
Why do a boy's testicles droop?
It is known that spermatozoa are formed in the seminiferous tubules of the testicles, which are necessary for fertilization of the egg for procreation. The peculiarity of sperm is that at high temperatures (above 34.5°C) they become non-viable. That is why the testicles in boys should be located outside the abdominal cavity.
The scrotum is a sac-like musculocutaneous formation that contains the testicles. The muscular layer of the scrotum is responsible for maintaining the optimal temperature of the testicles in the following way: at low ambient temperatures, the scrotum contracts, pressing the testicles closer to the body, and at high ambient temperatures, on the contrary, it relaxes.
IMPORTANT! Normal development of the testicles is possible only after they descend into the scrotum. An undescended testicle is smaller in size and lacks the processes of spermatogenesis.
Reasons why a boy's testicles do not descend:
- Hormonal disorders in a pregnant woman (diabetes mellitus, thyroid pathology);
- Pathology of testicular development in the embryo;
- Impassable or too narrow inguinal canal;
- Short spermatic cord, underdevelopment of testicular vessels;
- Insufficient development of the ligamentous apparatus;
- Functional immaturity of the fetus, premature birth;
- Injuries to the groin area after birth.
“Migrating” testicle – what is it?
Changes in air temperature in the room, crying or bathing the baby can cause the appearance of “migrating” testicles - a condition in which they rise into the inguinal canal. This phenomenon is caused by an increase in the tone of the muscle that lifts the testicle, and most often occurs at the age of 2-8 years. Testicular migration is called false cryptorchidism and, as a rule, does not require treatment.
The boy’s testicles have not descended into the scrotum: what to do?
Cases where boys' testicles descend later than usual are not uncommon. If the testicles “populate” the baby’s scrotum in the first six months of life, there is nothing to worry about.
It’s a completely different question when a six-month-old boy has one- or two-sided undescended testicles.
In this case, we will be talking about a planned surgical intervention, thanks to which it will be possible to place the child’s testicles where they belong.
True cryptorchidism is a condition in which, during a manual examination of the child, the doctor is unable to move the undescended testicle into the scrotum.
IMPORTANT! The only treatment for true cryptorchidism is surgery. Orchiopexy is an operation that involves lowering and fixing the testicle in the scrotum. Early orchidopexy (at the age of 9-18 months) avoids complications of cryptorchidism such as infertility, testicular torsion, malignant degeneration, etc.
If a boy's testicles do not descend at birth, parents should be extremely careful and observant.
If a boy’s testicles do not descend on their own, it is very important not to miss the time most favorable for surgical treatment of this pathology.
Of course, except in cases where a boy’s testicles descend after surgery, there are other methods of treating cryptorchidism, for example, hormone therapy, massage, therapeutic exercises, but their effectiveness is questionable and amounts to no more than 20%.
Source: https://nasha-mamochka.ru/o-detyah/do-goda/kogda-u-malchikov-opuskayutsya-yaichki/578
Age of testicular descent
Testicles develop in the womb
, are located in the abdominal cavity of the fetus. They remain there until the last weeks, and immediately before childbirth the process of their descent into the scrotum begins. The hormone testosterone is responsible for this movement.
Sometimes there are no newborn testicles in the scrotum. This is caused by the baby being born prematurely. The process of descent in most of these children is completed by 12 months. However, 20% of boys still have problems with this, in which case cryptorchidism is diagnosed. It can be one-sided or two-sided.
Cryptorchidism is translated from Greek as “hidden testicle.” This pathology is diagnosed at the time of birth, when one or both testicles are not found in the scrotum. Doctors often use the term “undescended testicle.” An anomaly when one testicle is missing at all is called monorchism.
.
Cryptorchidism involves the location of the testicles in the abdominal cavity, which causes overheating of the child’s reproductive system. If this temperature regime persists for a long time, then the formation of the testicles becomes abnormal. Further, this leads to problems with potency or the development of a cancerous tumor.
Features of therapy
Most experts recommend treating cryptorchidism in adults with surgery. In some cases, hormone therapy, microsurgery and laparoscopy are used. This or that treatment regimen is prescribed on a strictly individual basis, taking into account the general condition and age of the patient, the length of the spermatic cord, the location of the testicle, and the presence of complications. When should surgery be performed for cryptorchidism and should it be done at all? Only the attending physician can answer this question.
Modern medicine has the following methods of treating the above anomaly:
- Open surgery. Surgery for cryptorchidism is the most popular and effective treatment method. These manipulations can be performed in both childhood and adulthood under local anesthesia or general anesthesia. The essence of the operation is to move the testicle from places of pathological localization to the scrotum and fix it there. After performing this procedure, the man undergoes plastic surgery in the inguinal canal area. If surgery is not performed for cryptorchidism, then there is a high risk of developing oncogenic processes in the tissues of the organ. In this case, orchiectomy is indicated. In order to prevent the development of infectious complications after surgery, patients are required to be prescribed a course of antibiotic therapy.
Most clinicians recommend surgery when detecting cryptorchidism.
- Laparoscopy is a modern alternative to surgery. With its help, a high therapeutic effect is achieved, but at the same time, only three pinpoint scars remain on the patient’s body at the sites where special equipment was inserted.
Laparoscopy is an effective minimally invasive method for treating cryptorchidism
- Prosthetics. Indicated for adult patients who have had a testicle removed. This procedure helps restore the anatomical shape of the scrotum and relieve the patient’s psycho-emotional discomfort. Silicone implants are used as a prosthesis. Implants do not solve the problem of fertility; they perform only an aesthetic function.
Implants used in testicular replacement
- Drug therapy is aimed at restoring the functional activity of the diseased testis. There is a huge list of medications that the attending doctor can prescribe. The use of a particular medicine depends on the form of the pathology, the age of the patient and the etiology of the disease.
- Hormone therapy. In this case, human chorionic gonadotropin is most often used. The course of therapy lasts from 4 to 5 weeks. If the result is positive, the course of treatment must be repeated after three months.
Hormone therapy is most often prescribed when bilateral cryptorchidism is detected in men.
An increased dose of human chorionic gonadotropic hormone in cryptorchidism can provoke the development of side effects (hypertrophy of the penis and scrotum, intensive hair growth in the genital area, skin pigmentation). To restore the level of androgenic steroids in the patient’s body, doctors prescribe hormonal drugs (Testosterone, Nerobolil, etc.).
Symptoms of cryptorchidism, complications in children and adults
An undescended testicle is usually diagnosed immediately after birth when examined by a surgeon. Cryptorchidism in adults requires consultation with a urologist-andrologist. The disease is characterized by the following deviations:
- Shape of the scrotum - asymmetry of the scrotum or its underdevelopment and flattening (bilateral cryptorchidism);
- Nagging pain in the groin or abdomen, with the intra-abdominal location of the testicle, the pain increases with straining, constipation, tension in the abdominal wall, sexual arousal during puberty (adulting).
Normal testicular development and spermatogenesis take place only in the scrotum, the temperature of which is 1.5-3ºC lower than in the abdominal cavity. Therefore, the longer the testicle is located outside the scrotum and the higher the temperature of the internal environment of the body surrounding it, the higher the risk of rapid onset of changes in it at the morphological level.
Violation of the production of male hormones - androgenic hypofunction is detected during adolescence. In boys, secondary sexual characteristics develop slowly or are completely absent (with bilateral cryptorchidism): groin hair, facial hair.
Typically, adolescents with cryptorchidism have a high-pitched voice, their body type is female, and obesity often develops.
Incorrect placement of the testicle can lead to the development of the following conditions:
- infertility - due to a decrease in the number of healthy sperm;
- strangulation of the testicle in an inguinal hernia - requires emergency surgery;
- testicular torsion - compression of the spermatic cord, consisting of vessels and nerves, leads to rapid necrosis of the testicle;
- seminoma - testicular tumor occurs 35 times more often in patients with cryptorchidism;
- compression of the testicle by the pubic bone when it is located in the groin;
- psychological discomfort, feelings of inferiority and problems in the sexual sphere.
Causes of cryptorchidism
- The main reason for the development of cryptorchidism in boys is prematurity. If labor begins before 8 months of pregnancy, the testicles will not have enough time to descend.
- Another reason is the agenesis of Lockwood's tails - fibrous cords that pull the testicles to their final location. There are 5 tails on each side. And everyone is responsible for their own area.
- The movement of the testicles is affected by the concentration of hormones , intrauterine intoxication, the presence of mechanical obstacles, changes in intra-abdominal pressure, and the dynamics of the fetal intestine.
Treatment
Surgical treatment is the main method.
With timely treatment of cryptorchidism, it is possible to preserve reproductive function in 50-60% of cases with bilateral anomalies and in 80-85% with unilateral anomalies.
There are conservative and surgical treatment. The choice of treatment method is the prerogative of the doctor. Only he will determine the advisability of using hormone therapy, taking into account the type of cryptorchidism, the boy’s age, concomitant pathology, etc.
A conservative method of treating cryptorchidism is to prescribe hormonal drugs. Hormone therapy is used from 6 months to 2 years of age for a boy. This treatment is prescribed for bilateral anomalies, when the testicles are located close to the scrotum and for false cryptorchidism, when the testicles can be easily palpated. The effectiveness of the method is low - up to 30% of cases.
Gonadotropin-releasing hormone or human chorionic gonadotropin is used. It is usually administered twice a week intramuscularly, the course duration is up to 5 months. The treatment method is rarely used due to low effectiveness and the risk of side effects.
With hormonal therapy, the level of male sex hormones in the boy’s body increases, which should contribute to the correct formation of the scrotum and the descent of the testicles into it. Large doses of hormones can cause side effects such as an increase in the size of the penis and scrotum, prostate gland, growth of pubic hair, etc. After reducing the dose, all these effects disappear.
If after hormonal therapy the testicle does not descend into the scrotum, surgery (orchiopexy) is performed.
Surgical treatment is used in most cases of cryptorchidism. If spontaneous testicular descent has not occurred by one year, the child will need surgical treatment.
Orchiopexy is a simple operation, but it requires highly qualified and expert work of the surgeon. Children tolerate it well, and it has a low rate of postoperative complications.
During the operation, an incision is made in the groin area. Through it, the testicle is lowered into the scrotum and fixed there. If there is an inguinal hernia, it is also eliminated. The operation is performed without penetration into the abdominal cavity, under general anesthesia or local anesthesia.
A simple operation (fixation of the testicle) is necessary when the testicle migrates (when it either descends into the scrotum or rises again to the groin).
In addition to the traditional method of treating cryptorchidism, the laparoscopic method can also be used if it is necessary to remove the testicle from the abdominal cavity. Laparoscopic surgery can be performed in one or two stages. In a 2-stage operation, the testicle is gradually prepared for descent into the scrotum.
In some cases, the testicle is removed. Indications for removal are:
- testicular underdevelopment;
- complex fusion of the testicle with other tissues;
- complex torsion of the spermatic cord.
Complications after any such operation are extremely rare. They are more often associated with concomitant pathologies in the baby. In some cases, a hematoma or inflammation may form along the suture.
In rare cases, atrophy of the testicle relegated to the scrotum may occur. Sometimes surgical treatment is combined with hormonal treatment to restore the function of a descended testicle.
The boy is discharged three days after the operation. It is recommended to protect the child from jumping and sudden movements, from falling and running. During the recovery period, massage and therapeutic exercises, physiotherapy and water procedures may be prescribed.
After the operation, the doctor examines the child weekly in the first month, and then monthly for six months. Subsequently, observation by a urologist or andrologist is carried out every 6 months.
Orchiopexy at an early age for a boy has the following advantages:
- preventing infertility;
- simultaneous elimination of inguinal hernia;
- reducing the risk of developing a malignant tumor;
- prevention of testicular torsion and trauma.
Why may boys' testicles not descend?
Men always react painfully when they have problems and malfunctions in their reproductive and reproductive systems.
Therefore, from childhood, you need to pay attention to the boy and, if necessary, have an examination by a urologist so as not to miss pathology. A common pathology that can occur in a child at an early age is testicular prolapse. It is very important to know that this disease can lead to serious problems in the future. Especially at a time when the boy wants to become a father.
How does this happen?
The genital organs of the embryo begin to form in the second month of pregnancy . This is a very important moment for the development of a child. Therefore, if a woman does not lead an active and healthy lifestyle, the fetus will begin to develop abnormal developments of the genitourinary system.
During pregnancy, the testicles are located in the peritoneum or groin area. They descend into the scrotum just before the baby is born. This is the normal position of the testes. When the testicles are located outside the scrotum, it is called cryptorchidism.
For what?
As you know, sperm are formed in the testicles, which are necessary for fertilizing the egg and conceiving a child. At temperatures above 34 degrees, sperm lose their properties and die. Therefore, the testicles are located not in the abdominal cavity, but in the scrotum.
The scrotum is a muscular sac that contains the testes. The muscle layer is responsible for maintaining a special temperature in the scrotum.
At low temperatures, the scrotum contracts, and the testicles are pressed closer to the body, and, conversely, at high temperatures, relaxation occurs, and the testicles descend into the scrotum. A testicle that has not descended is smaller in size and sperm cannot develop in it .
Why does pathology appear?
There is no reliable evidence why the testicles do not descend into the scrotum.
There are several reasons for the development of this pathology:
- Failure of a pregnant woman to follow a healthy lifestyle;
- Taking antibacterial therapy;
- Increased pressure in the peritoneum;
- Hormonal disorders;
- Chronic processes in a pregnant woman: diabetes, dysfunction of the thyroid gland and pituitary gland;
- Prematurity;
- Narrowing of the inguinal canal;
- Anomaly in the development of the testicular ligament.
How is cryptorchidism diagnosed in infants?
Cryptorchidism can be detected quite easily by palpation. But for an accurate diagnosis, it is necessary to undergo additional examination. After birth, all newborn boys are examined by a doctor to detect this disease.
When examining the scrotum, the doctor determines at what stage the descent of the testicles is. A small child is prescribed to undergo an ultrasound of the pelvic organs.
It is believed that within a year of life, the testicles can descend into the scrotum on their own. When during this time the testes have not taken their place in the scrotum, the child is prescribed surgical intervention. Urologists recommend the operation be performed up to five years of life.
Alternative judgments
According to many doctors, when the testicles have not descended into the scrotum, this is not a reason to panic. Sometimes in newborn children, internal organs can take a wandering position. For example, the testicles may descend into the scrotum and rise back up to the groin.
The reasons for such actions are not fully understood. They say that special muscles are to blame, which should protect the baby’s delicate organs. With a slight touch to the testicles, they rise to the groin. This also happens at low ambient temperatures.
Optimal timing
The most appropriate time for the testicles to descend into the scrotum is the last days of gestation. The testicles of almost one hundred percent of newborns occupy their correct, physiological position when the baby is born at the specified time. In premature babies, they do not go down in all of them.
It is believed that by the age of one year the testicles should descend into the scrotum on their own without treatment, massages or other actions. This is the final date for them to take their position.
When the temperature is low, the testes are in the groin and do not want to descend into the scrotum. Sometimes light massage movements and heat can return the testicles to their place. You can also use relaxing and warm baths.
Is it necessary to have surgery?
The doctor observes the child for up to a year, if he is suspected of having the disease cryptorchidism. If testicular descent does not occur, then surgical intervention is necessary. Typically, non-prolapse of the testes indicates that previously prescribed procedures did not produce the desired result.
Treatment and observation are carried out by an andrologist and pediatrician, as well as a pediatric endocrinologist. Some doctors recommend surgery when the child reaches ten months. Before this period, the prolapse may go away on its own. An alternative to surgery is conservative treatment. The child is prescribed an injection of human chorionic gonadotropin.
This is a hormonal medication that can help the testis descend into the scrotum. This treatment is effective only in early childhood.
When prolapse does not occur before puberty, hormonal therapy cannot be performed. During this period, gonadotropin levels in the boy’s blood naturally increase. During surgery, the testicle is lowered into the scrotum. During surgery, a biopsy is taken so as not to miss a neoplasm or gonadal dyskinesia.
Why is timely treatment necessary?
If the parents refuse the operation or it is performed too late, the child may experience necrosis or degeneration of the organ into a malignant tumor. Then the testicle is simply removed. During the operation, the question arises of transplanting a donor testicle or introducing an implant for cosmetic correction.
Untimely treatment leads to testicular development under unfavorable conditions. This causes infertility and poor sperm maturation.
Cryptorchidism in men
Cryptorchidism in adult men is the abnormal position of one or two testicles. With normal development, the testicles descend into the scrotum before or after childbirth. But sometimes they stop the descent process in the abdomen or groin.
Symptoms:
- Absence of a testicle in the scrotum;
- The presence of asymmetry;
- Underdevelopment of the scrotum;
- Pain at the site of abnormal descent of the testicle;
- Disturbance in the production of male hormones.
There are two types of cryptorchidism:
- True cryptorchidism . You can easily feel the testicle, but lowering it is not possible due to underdevelopment of the right or left side of the scrotum:
- False cryptorchidism or migrating testicle. When it is warm, the testicle is located in the scrotum, and when the temperature drops, it rises to the groin. This also happens when muscles relax and tense. There is no need for treatment here;
Types of cryptorchidism:
- Inguinal. The testicle is located under or above the inguinal ring;
- Abdominal. The testicle is found using CT or ultrasound results. With this type of cryptorchidism, men experience pain in the testicular area. This is the most common form of the disease;
- Ectopic testicle. With this pathology, the testicle descends not into the scrotum, but into the groin, the base of the penis.
Cryptorchidism is a disease of early childhood, but sometimes men develop pathology as a result of injury or expansion of the inguinal ring.
What to do?
Treatment is prescribed only after a complete examination of the patient. When making a diagnosis and studying the tissue of the prostate and pelvic organs, the doctor prescribes a comprehensive treatment.
Features of the treatment process
The main treatment for the patient is surgery.
Therefore, to make an accurate diagnosis, the patient is prescribed to undergo the following diagnostics:
- Ultrasound of the pelvis;
- MRI;
- CT;
- Scintigraphy;
- Angiography;
- Thermography;
- Probing.
Treatment method:
- Operation;
- Laparoscopy;
- Prosthetics;
- Use of medications;
- Hormonal therapy.
Cryptorchidism in men is an obstacle to conceiving a child and the development of infertility. If you do not receive treatment in time, the disease can develop into a malignant tumor.
Bottom line
Cryptorchidism is a serious disease that requires diagnosis and timely treatment. Testicular descent occurs just before childbirth or after it until the first year of life. When this does not happen, a child under five years of age undergoes surgical treatment to remove the testicle.
Also, a good alternative to surgery is conservative treatment, which is based on the administration of the human chorionic gonadotropin hormone. After such an injection, the testicle may descend into the scrotum on its own. But such treatment can only be carried out at an early age; in adolescence, the content of male hormones is already increased.
The absence of a testicle can lead to:
- impaired sperm formation;
- infertility;
- development of malignant tumors.
Modern diagnostic methods make it possible to find a testicle in the abdominal cavity or groin and prescribe appropriate treatment. You can easily feel a missing testicle in a newborn. There is no reliable information why a child’s testes do not descend on their own. The reproductive organs of the embryo begin to form in the second month of pregnancy.
During this period, it is very important for a woman to lead a healthy lifestyle and not take antibiotics. Otherwise, it will have a detrimental effect on the development of the child’s organs. Sometimes the testicles do not descend due to underdevelopment of one side of the scrotum. Nowadays, an implant or transplant of a donor testis can be used during the operation.
Source: https://kakbog.com/bolezni/opuschenie-yaichek.html
Complications of cryptorchidism
Undescended testicle into the scrotum is not only a cosmetic problem. If left untreated, this anomaly can cause a number of complications.
In approximately 70% of cases, the testicles descend spontaneously into the scrotum during the first months of a boy’s life. If they have not subsided by 6 months, then it is necessary to decide on the treatment of the child in order to avoid complications.
Such complications may be:
- impairment of reproductive function (infertility) in the future: degenerative changes occur in the undescended testicles within 6-12 months due to exposure to temperatures in the abdominal cavity that are higher (1.5-2.5°C) than in the scrotum. The longer the testicle is outside the scrotum, the more spermatogenic (fertile) function suffers. In addition, changes in one testicle may trigger autoimmune processes that will lead to damage in the second (even normally located) testicle. The higher the testicle is located in the abdominal cavity, the faster irreversible pathological changes will develop in it.
- The production of hormones by the testicles (androgenic function) is also gradually disrupted: there is a tendency towards excess body weight, secondary sexual characteristics develop untimely or insufficiently. Hair practically does not grow in the groin area, the beard and mustache grow slowly, the pitch of the voice is high; boys have an effeminate physique and they develop impotence in the future.
- Possible malignant degeneration of the tissue of the undescended testicle; the probability of developing testicular cancer (seminoma) according to various authors is from 10 to 35 rubles. higher than in its normal location.
- Torsion or inversion of the testicle in the inguinal canal, requiring emergency surgery.
- Strangulation of the inguinal hernia, often accompanying cryptorchidism.
- Injury to the testicle located in the groin, thigh, perineum.
Norm
Until the 3rd month of the antenatal period, the testicles are located under the lower poles of the kidneys and are located retroperitoneally. Then they begin to move towards the scrotum, protruding the sheet of peritoneum forward and being surrounded by it. Eventually the testicles become wrapped in peritoneum, which later becomes one of the membranes.
Then the testicles enter the inguinal canal, move along it and exit through the inguinal ring into the scrotal cavity. By the 8th month of intrauterine development, the testicles reach physiological localization.
Prognosis, complications
Histological studies have shown that even at the stage of intrauterine development, cryptorchidism provokes degenerative changes. The prognosis is based on the height of the testicle in the abdominal cavity and the duration of its presence there. The temperature in the abdominal cavity is approximately 2 degrees higher than in the scrotum, which negatively affects spermatogenesis. The less time the testicle remains in the abdominal cavity and is located lower, the less the effect of elevated temperature on reproductive function.
The following complications also arise against the background of cryptorchidism:
- disruption of hormone production - androgenic function;
- violation of the timely and complete development of secondary sexual characteristics: complete or partial absence of hair in the groin and pubic area, slow and weak growth of mustache and beard, high-pitched voice;
- hypospadias is a malformation of the genitourinary system, implying the opening of the external opening of the urethra on the lower surface of the penis;
- dropsy of the testicular membranes;
- femineity;
- development of impotence;
- increased risk of testicular malignancy;
- testicular inversion;
- testicular injury.
What parents need to know about cryptorchidism in children, says pediatric urologist Karaman Abramov:
Cryptorchidism is characteristic only of the male sex and is a congenital pathology. In most cases, the disorder resolves on its own during the first year of the child’s life. For other patients, treatment is necessary, which can be medication (hormonal therapy) or surgery. The operation is carried out using different methods.
Types of disease
There are three types of cryptorchidism, differing in the location of the testicles: true, false and ectopia.
True cryptorchidism
In babies, the undescended testicle is located in the groin or abdominal cavity. To determine the location of the testicle, there is no need for special types of diagnostics; it is easily determined by palpation with pressure in the groin area. If the testicle is located in the pelvis, it cannot be identified by touch. In this case, the most informative method will be ultrasound. The idea that testes can burst is wrong.
False cryptorchidism
False cryptorchidism is characterized by the fact that the testicle periodically descends into the scrotum, while occupying the correct position, the same as in children with normal physiological development. This process is due to the fact that the muscles responsible for raising the baby’s testicles tense up from time to time. The cause may be severe stress or hypothermia.
This form of the disease is observed in boys under 5 years of age. Treatment of this pathology is not necessary, since the testicle rises on its own and is fixed in the scrotum. By the onset of puberty in adolescents, false cryptorchidism completely disappears.
Ectopia
Ectopia differs from other types of pathology in that it occurs in the fetus during intrauterine development. The testicles do not descend into a sac, but settle in the abdomen, thigh, or groin. As practice shows, the testicle can rise again. In most cases, this is due to previous injuries, but the descent of the testicles into the abdominal or groin cavity can also be caused by improper development of the spermatic cords.
There are bilateral and unilateral cryptorchidism. In the first case, both testicles do not descend in boys, and in the second, only one. Unilateral cryptorchidism can be left-sided or right-sided.
INTERESTING: what is hypospadias in newborn boys?
When do boys' testicles descend?
After the birth of the baby, parents try to protect their child as much as possible from various types of ailments and pathological processes. Equally important is the development of the genital organs. The question often arises: “At what age do boys’ testicles descend?”
The process of proper formation of a boy's genitals
All children develop at their own pace, for some the development is a little delayed, for others, on the contrary, it happens more quickly. But despite the differences, there are certain norms. If they are rejected, doctors are already looking for the cause of the disease and making a diagnosis.
In most newborn boys, the testicles descend into their biological place from birth until 6 weeks. It should be emphasized that this is not what happens to all children. In some cases, a child’s testicles do not descend until 6 months, and sometimes even up to 9 months after birth.
Until this age, parents should not panic too much; it is enough to simply keep the process under control and visit children's doctors in a timely manner for a routine examination.
When a child becomes older than 9 months of age, but prolapse of the organ into the scrotum has not yet been detected, it is necessary to urgently consult a doctor and identify the cause of the pathological process. The examination is carried out by a pediatric surgeon or urologist.
It is very important to carry out the necessary surgical operations in a timely manner. The intervention should be from 9 to 18 months of age of the baby. If this time is missed, pathologies and disturbances in the development of the reproductive system will begin to develop. Common problems include:
- impaired sperm production;
- infertility;
- malignant processes in the reproductive system (rare).
If the child’s testicles do not descend, the doctor will prescribe a planned operation to force the organ into the right place. After surgery, parents should know how to properly care for their child and follow the doctor’s recommendations.
As he grows up, it is imperative to teach the boy to independently examine the genitals and respond to any changes in the reproductive system. These include changes in the size of the penis and scrotum, as well as fluctuations in the shape of the genitals.
Until adulthood, these aspects should be monitored by parents and, if necessary, visited by doctors.
"Walking" gland
In medical terminology, there is the term “walking testicle”. As a result of the influence of certain factors, the boy’s iron may either descend into the scrotum or rise into the inguinal canal. A boy’s testicle does not descend when it’s cold, but when it gets warm, the glandular organ comes back into place.
Such a process in medicine is not considered a disease, but is a normal physiological phenomenon. Parents should not panic. It is necessary to learn to understand when a child’s testicle “walks” and in what situations it is a pathological process.
In babies, the “walking” organ can be identified by the following signs:
- When swimming in warm water, drooping occurs;
- When the baby squats, the organ falls into place;
- When exposed to warm hands on the child’s scrotum;
- When a child sits down to play and spreads his legs to the sides for a stable body position.
If at these moments the boy’s testicles do not descend, then you should contact a pediatric urologist as soon as possible. A “walking” gland can only be observed until the age of 9. Around the age of 8–9 years, the child begins to experience hormonal activity, which leads to an enlargement of the organ and a gain in strength.
As a result, the testicles descend into the scrotum and no longer rise into the inguinal canal. In this case, no treatment is required. In exceptional situations, the organ remains mobile even in older men, while the spermatogram and functionality of the reproductive system are noted to be within normal limits.
In any case, the doctor must monitor the baby’s health status over a long period of time. Regular examinations must be carried out every six months.
Note!
In some situations, a “walking” testicle can get stuck in the inguinal canal. In this case, surgical intervention is mandatory.
Causes of the pathological process
In babies, the testicles are located in the abdominal cavity, near the kidneys. They then descend through the inguinal canal into the scrotal cavity. Parents can check the situation themselves. It is enough to simply feel the scrotum with your hands.
Often the organ does not descend or only one testicle descends, while the second wanders. This process is diagnosed as cryptorchidism. Doctors can make this diagnosis immediately after the baby is born. Using ultrasound, the location where the organ is stuck is determined.
Among the causes of this pathology in a child are the following negative factors:
- Parental smoking;
- Drinking alcohol during pregnancy;
- Maternal hormonal imbalance;
- Pathologies of the endocrine system;
- Taking medications;
- Increased sugar levels;
- Metabolism;
- Problems with digestive function.
The above factors cause problems not only with the gland, but also with the spermatic cord, inguinal canals, and penis.
Therefore, to prevent problems with the child’s health, parents should take a responsible approach to pregnancy planning. First, get rid of bad habits and undergo a health diagnosis.
Pregnancy planning is a responsible approach for both parents to the birth of a baby.
Source: https://anatomiy.com/ne-opuskayutsya-yaichki-u-rebenka.html
Surgery
Indications for surgery for cryptorchidism
- undescended testicle – true cryptorchidism
- spermatic cord torsion
- testicular strangulation
- inguinal hernia
- ectopia testis
- testicular hypotrophy – disruption of tissue nutrition and decrease in its mass.
At what age is it better to have surgery? Contraindications to surgery
- severe chronic pathologies of the heart, liver and kidneys
- bleeding disorder
Types of operations for cryptorchidism
- Simultaneous operation according to Schumacher - Petrivalsky. One incision is made in the inguinal canal, providing access to the testicle, and the second on the scrotum. The spermatic cord is lengthened, freeing it from the peritoneum and fibrous cords. Using a clamp, the testicle is lowered into place and fixed, suturing it to the wall of the scrotum. Both wounds are sutured. During the operation, a testicular biopsy is performed. If the examination reveals signs of malignancy, atrophy (decrease in volume) or necrosis (death of cells), then the testicle is removed. If cryptorchidism is accompanied by an inguinal hernia (20-80% of cases), then during the operation it is sutured.
- Two-stage reduction of the testicle with its fixation to the fascia of the thigh or staged movement of the testicle. This operation is performed if the doctor discovers that the spermatic cord is short - it is stretched and does not allow the testicle to descend into the scrotum. In this case, the gland is lowered in stages, lengthening the spermatic cord. At the first stage, the inguinal canal is opened, the testicle is released, and the spermatic cord is lengthened. An incision is made on the scrotum and a bed for the testicle is formed. An incision is made on the thigh and the fascia lata of the thigh is exposed, to which the testicle is sutured by the tunica albuginea. Then the edges of the incision on the thigh and scrotum are sewn together. After 2-4 months, the second stage of the operation is performed. During which the testicle is moved into the scrotum.
Laparoscopic operations. For ectopia. Preparation for surgery for cryptorchidism.
- Examination by a therapist to identify concomitant chronic diseases (sinusitis, tonsillitis, bronchitis), which can cause postoperative complications.
- A week before the proposed operation, stop taking aspirin and other blood thinning drugs that can cause bleeding.
- Blood, stool and urine tests.
- To clarify the location and condition of the testicle, an ultrasound or MRI is repeated.
- Consultation with an anesthesiologist to identify risks that may arise during anesthesia.
- The evening before surgery, take a shower. Adult men should shave their groin hair.
- Last meal in the evening, 8-10 hours before surgery. This is necessary so that the patient can tolerate anesthesia more easily.
Rehabilitation after surgery for cryptorchidism
- In the first days after surgery for testicular prolapse, antibiotics are prescribed to prevent complications.
- For pain relief, non-steroidal anti-inflammatory drugs are prescribed: Nurofen, Paracetamol.
- You can apply an ice pack wrapped in a towel over the bandage. A cold compress relieves soreness and swelling.
- The first 10 days require daily dressings. During which medical personnel assess the condition of the wound and treat it with antiseptic agents. Follow your surgeon's recommendations strictly. Do not apply any ointments to the wound, do not smear it with iodine without a doctor’s permission.
- Make sure that the incision area remains clean and dry at all times. The skin around the seam is wiped with gauze wipes soaked in soapy water and then dried.
- On days 7-12, the sutures are removed and the wound is continued to be treated with peroxide to remove crusts.
- Walking and light exercise are allowed for days 3-5. They improve blood circulation and the emotional state of the patient. Active actions must be avoided so that the suture does not come apart and bleeding begins.
- Physical activity is allowed one month after the operation.
- Adult patients need to postpone sexual activity for 3-4 weeks. Otherwise, painful sensations during sexual intercourse are possible.
- temperature rise above 37.5
- heavy bleeding from the wound
- wound discharge
- loosening or splitting of seams
- pain, redness and swelling around the stitch
Disease prognosis
When boys' testicles descend: reasons for non-descent, diagnosis and treatment
Article last updated: 05/03/2018
Testicles (testicles, gonads) are organs of the male reproductive system, the main functions of which are the formation of sperm, the production of testosterone and its derivatives.
When do boys' testicles descend?
The fetal testicles begin to descend in the womb, in the 6th month of pregnancy.
This process ends before childbirth or immediately after birth.
The testicles may descend in the first year of the baby's life. In this case, the child should be observed by a urologist.
If the testicles do not descend into the scrotum, we are talking about pathology - cryptorchidism and ectopia.
The descent of the testicles can be thought of as a route with stops. If the testicle is stuck on one of them, this pathology is called cryptorchidism. A pathology in which it deviates from the route is called ectopia.
From the fetus:
- Genetic mutations.
- Mechanical obstacles along the movement of the testicle - connective tissue cords of the inguinal canal, short testicular artery, short spermatic cord, narrow inguinal canal, disturbance of intra-abdominal pressure.
- Endocrine pathology. These are hypothalamic-pituitary disorders of the fetus, a violation of the synthesis of testosterone by the fetal testicles.
From the mother's side:
- Endocrine pathology - diabetes mellitus, pathologies of thyroid function, low production of gonadotropins at the end of pregnancy.
- The use of non-steroidal anti-inflammatory drugs (NSAIDs) - Paracetamol, Aspirin, Ibuprofen at the beginning of pregnancy.
If you are planning a pregnancy or are already expecting a child, monitor your blood glucose levels and thyroid hormone levels. Also avoid taking NSAIDs.
- The main sign of cryptorchidism and ectopia is the absence of one or two testicles in the scrotum, which is determined by palpation. If it seems to you that the child is missing a testicle or testicles in the scrotum, carry out several actions: touch the scrotum with warm hands; the testicle is defined as an elastic oval body. During this manipulation, the baby should be calm. If you can’t find it, watch your child while bathing. In warm water, the muscle that lifts the testicle (creamaster muscle) relaxes, and it descends into the scrotum.
- With unilateral cryptorchidism and ectopia, the scrotum is asymmetrical; with bilateral cryptorchidism, both halves are underdeveloped.
- In 70% of cases, the boy’s testicle hurts during physical activity or palpation.
These diseases can be painless. Therefore, parents and doctors should pay close attention to the presence of testicles in the scrotum of newborn boys.
The main research method is palpation. For a non-palpable testicle, ultrasound is used. If the testicle is absent even on ultrasound, diagnostic laparoscopy is performed.
Treatment
The most effective surgical treatment for cryptorchidism. It is carried out when the child is between one and a half years old. Before the operation, the baby is observed by a pediatric urologist.
As a preparation before surgery, hormonal therapy can be carried out.
Complications
Correct development of the sex glands is possible only in the scrotum. Other cases lead to various complications, including:
- disturbance of spermatogenesis;
- testicular torsion;
- traumatic orchitis (testicular inflammation);
- testicular strangulation;
- testicular cancer.
Violation of the spermatogenic function of the testicle occurs with prolonged cryptorchidism. It has been proven that the death of testicular tissue begins at the age of two. In patients with operated bilateral cryptorchidism, the spermatogram is often abnormal. There are few or many sperm with an irregular structure, their motility is reduced.
Testicular torsion is more common at 1 - 3 years and at 10 - 15 years. The reason is excessive mobility and violation of its fixation.
Sometimes the testicle lies in the inguinal hernia and is strangulated along with it.
Traumatic orchitis with cryptorchidism develops as a result of generic grass in newborns and is called idiopathic testicular infarction.
The above conditions have a similar clinical picture and are called “acute scrotal syndrome”.
The risk of developing cancer of an undescended testicle is 20 times higher. And it does not depend on whether treatment was carried out or not.
Patients with operated cryptorchidism should be observed by a urologist in both adolescence and adulthood.
If the operation is performed on time, the prognosis is often favorable.
Pseudocryptorchidism, or wandering testicle
With pseudocryptorchidism, the scrotum is symmetrical. On palpation, the testicle easily sinks to the bottom of the scrotum, but due to the strong cremasteric reflex it returns to its original position. This condition goes away during puberty.
With pseudocryptorchidism, the functions of the boy's testicles are not impaired.
Pain in the testicles. Causes and manifestations
Testicular pain is a reason to immediately consult a doctor.
Reasons why boys have testicular pain:
- testicular torsion;
- strangulation of the testicle in the inguinal hernia;
- traumatic orchitis;
- inflammatory orchitis.
These conditions have a similar clinical picture (signs) and are united by the term “acute scrotal syndrome.”
The clinical picture includes the following symptoms:
- sharp pain in the scrotum and testicle, radiating to the groin area;
- swelling of the scrotum, its hyperemia (redness) on one or both sides;
- enlarged, dense testicle;
- fever, nausea, vomiting, pale skin.
In children under one year of age, fever, vomiting, loud crying, and breast refusal come first.
Let's look at diseases that cause pain in the testicles.
Testicular torsion and strangulation in an inguinal hernia are described above.
In traumatic orchitis, the severity of the lesion depends on the strength and type of injury. There is a bruise, dislocation, rupture and separation of the testicle.
If there is a bruise, the pain goes away after a while, bruising, hyperemia, and swelling are visible on the scrotum. In case of severe injury, vomiting and fever may occur. Upon examination, a hematoma (bruise) of soft tissues, hyperemia, swelling, and tenderness of the scrotum are visible. The testicle is enlarged and painful.
If, after a blow or fall, a boy complains that his testicle hurts, and there are bruises, a hematoma, or a swollen scrotum in the scrotum area, he should immediately consult a surgeon or urologist. With a minor injury, the pain quickly subsides and there are no visible changes.
Inflammatory orchitis occurs more often in newborns, and the cause is the penetration of infection through the umbilical vessels. In children over 10 years of age, orchitis is a complication of mumps (mumps) and occurs on the 3rd to 12th day of illness. Against the background of this disease, pain in the testicles appears in boys.
Torsion, strangulation of the testicle, rupture, and separation of the testicle are treated surgically.
For inflammatory orchitis, bruise and dislocation, treatment is conservative. It includes bed rest, a fixing bandage on the scrotum, antibacterial therapy, anti-inflammatory drugs, and glucocorticoids.
In children who have suffered from diseases associated with the “acute scrotum” syndrome, it is necessary to examine sperm in adolescence.
Symptoms
If there are any signs of illness, do not risk your child’s health - consult a doctor! Choose a specialist yourself or contact our help desk. The best doctors in Moscow are ready to see you:
289 pediatricians, 28 andrologists, 11 of them accept house calls.
Visually, the disease is manifested by the absence of testicles on one or both sides. Usually the missing testicle can be felt closer to the groin or thigh. Then additional examinations are prescribed, based on the results of which a decision is made on surgical intervention. If the organ is completely absent on one or both sides, they speak of mono- or anorchism, and this condition, unfortunately, cannot be treated.
Over 55% occur with right-sided cryptorchidism, when testicular descent is found only on the right side. In approximately a third of cases, the left-sided form is diagnosed. No patterns have been identified that cause omission on one side or another. About 10% of cases occur with bilateral cryptorchidism, in which both testicles remain in the abdominal cavity.
What it is
Cryptorchidism is the failure of the testicles to descend into the scrotum. In this case, the testicle may be located somewhere near the place where it should be normally, for example, in the peritoneum or inguinal area, mainly in the area of the inguinal canal. Sometimes the gonad of boys generally “deviates from the course” and leaves the inguinal canal, remaining subcutaneously in the thigh, pubis, and perineum.
If the baby is very premature and his birth weight is about 1 kilogram, then doctors will detect cryptorchidism in him with almost one hundred percent probability. In more than half of the facts, the “lost” testicle can be felt through the skin. However, sometimes this cannot be done, since there is a congenital developmental anomaly - the complete absence of one or two gonads in a child.
Why the testicles may not descend
In this section, we will look at the reasons why the process of testicular descent in boys may be disrupted:
- disturbances in the functioning of the hormonal system of the expectant mother or embryo - this is improper functioning of the thyroid gland, diabetes mellitus, and the like;
- inhibition in the development of the testicles of the embryo, which must be determined in the early stages;
- the inguinal canal is very narrow or completely impassable;
- inhibition in the development of testicular vessels or undeveloped spermatic cord;
- deviations in the development of the ligamentous apparatus;
- early labor (when a woman gives birth before the scheduled time) or functional inability of the fetus;
- damage to the groin area after birth;
- it can also be caused by the development of Down syndrome or a mutation of the GTD gene.